Clinical Evaluation of Diabetic Eye Disease
Diabetes is a systemic disease which damages blood vessels in the eye and, if unabated, can cause blindness. New data is now available which suggests that vision loss related to early vascular damage in the eyes of diabetic patients can be detected by contrast sensitivity evaluation. Even in patients who have 20/20 or better acuity, contrast sensitivity has been shown to be decreased. There are two key criteria to evaluate abnormality of contrast sensitivity in diabetic patients; below the normal range and asymmetry between eyes.
Below the Normal Range
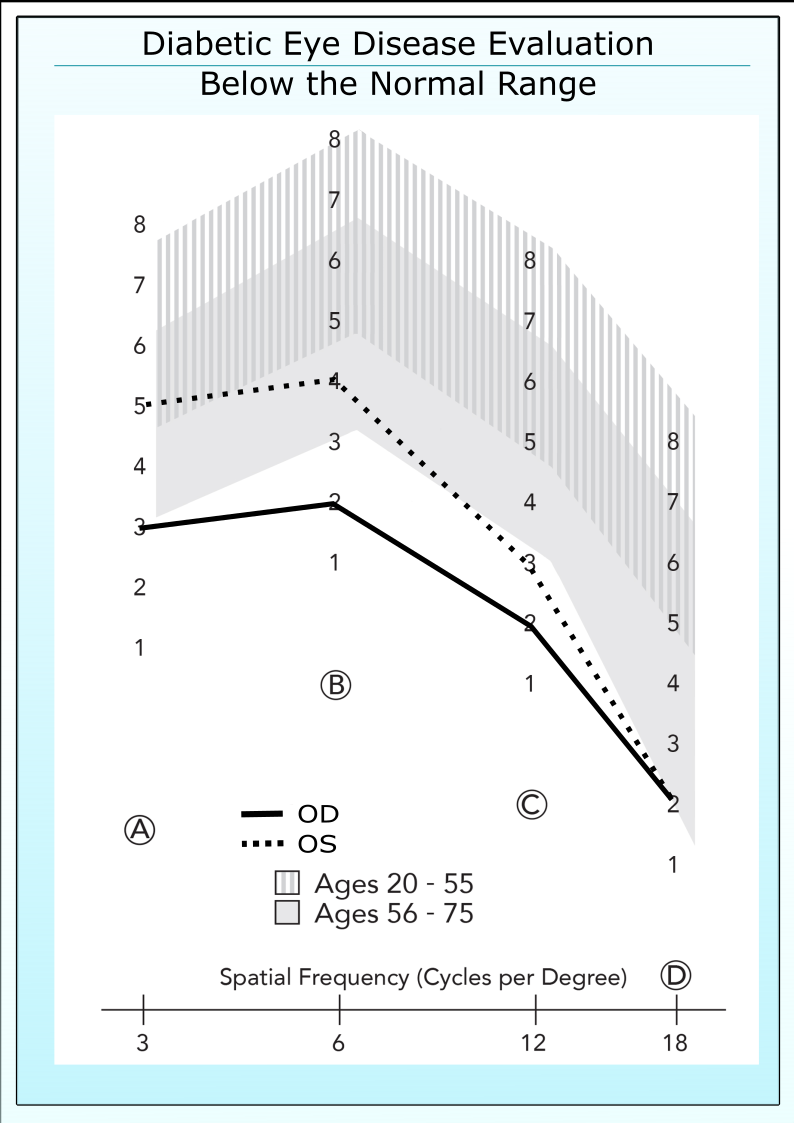
If a patient has good acuity, 20/30 or better, then he or she should have good contrast sensitivity. One hallmark of diabetic eye disease is that patients fall outside the normal range (patch 3 or below in either Row B or Row C), even when acuity remains normal. The example below shows a 33 year old diabetic patient with 20/20 acuity. The contrast sensitivity is below the normal range even though this patient had no apparent retinopathy.
Asymmetry Between Eyes
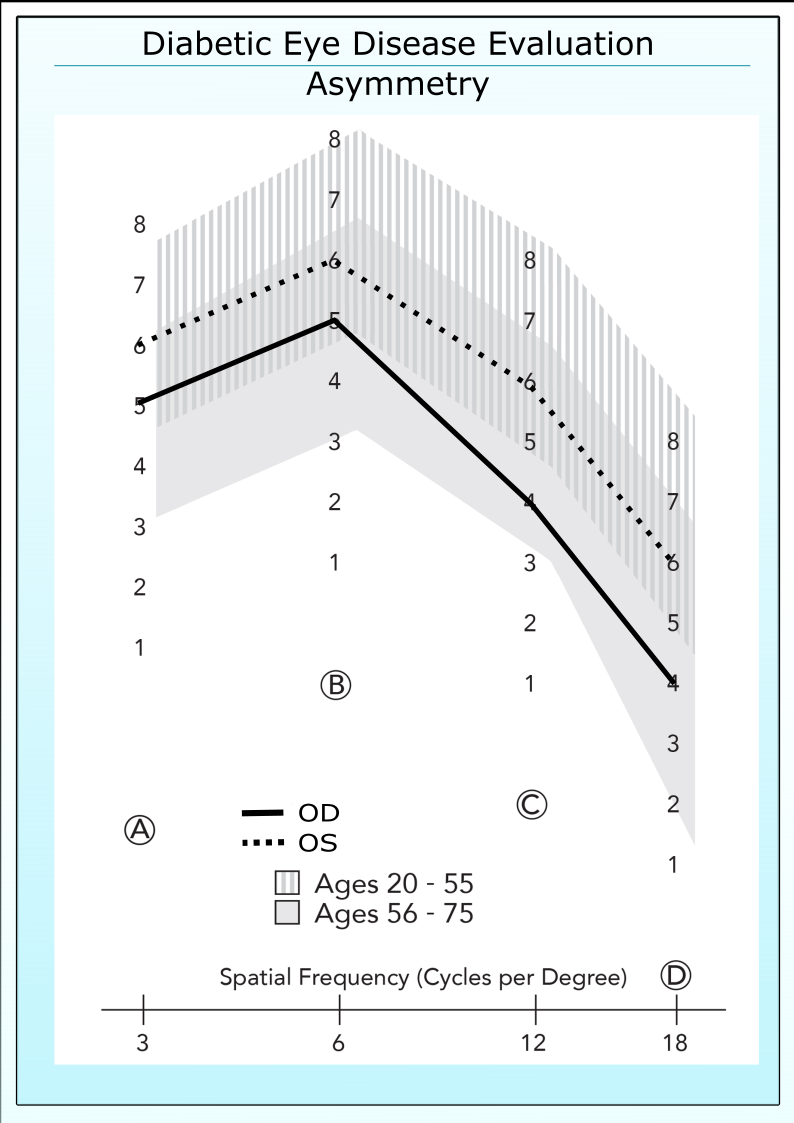
If a patient has the same acuity in both eyes, then contrast sensitivity should also be the same. A difference between eyes or asymmetry in CS is an early indicator of disease progression. The presence of a difference of 2 contrast levels (.3 log units) or more between eyes indicates that a significant loss in contrast sensitivity, even if both eyes are inside the normal range.
Relationship to Vasculature of the Diseased Eye
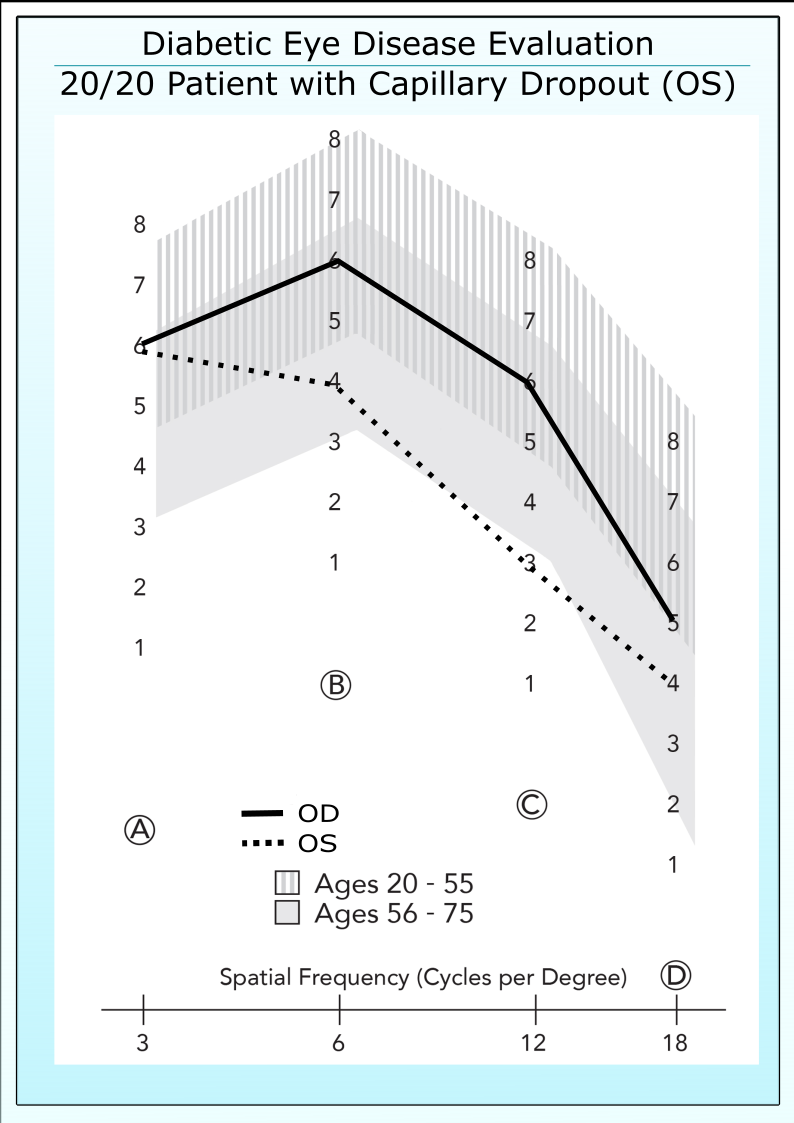
Published data by Arend et al (Arend et al. Invest Ophthalmol Vis Sci. Aug 1997) demonstrates that diabetic patients with good acuity may display vasculature damage in the retina, such as capillary drop-out or expansion of the foveal avascular zone.
These same patients display reductions in contrast sensitivity which are correlated to the level of vascular damage. Importantly, these retinal defects cannot be directly detected without the patient undergoing fluorescein angiography, an invasive procedure. These results suggests that contrast sensitivity may aid in screening patients and determining whether an angiogram is warranted.
Control of Treatment
Recent evidence (Mangouritsas et al. Ophthalmologic. April 1995) shows that contrast sensitivity falls during periods of artificially induced hyperglycemia in insulin dependent diabetic patients. These results suggests that contrast sensitivity may have a possible role in evaluating the treatment control of diabetic patients.
Refractive Error Must Be Corrected When Testing
It is very important to remember that the patients should be evaluated with best correction. Contrast sensitivity is very sensitive to refractive error. If a patient exhibits a deficit in contrast sensitivity, the correction of the patient should be re-checked to insure that the measured vision loss is not due to refractive error.
Most Useful in Younger Patients
Contrast sensitivity is most useful in the evaluation of diabetic eye disease in younger patients. Contrast sensitivity can be dramatically affected by the presence of cataracts or other eye anomalies. Younger patients are less likely to have other contaminating vision problems and as such the loss in contrast sensitivity can be used to assess the progression of diabetes. Remember to compare individual contrast sensitivity scores to the normal values of a similar age group. Old and younger normal values are available in another part of this website.
Featured Product
CSV-2000
CSV-2000 The first and only all-in-one digital vision testing device that offers the full range of vision tests, along with STANDARDIZED contrast sensitivity, glare and visual acuity.
Over the last 20 years, VectorVision testing equipment has become the worldwide benchmark for standardized contrast sensitivity, glare and ETDRS acuity testing.
Read our Reviews